H5N1 pig infection: first US case detected
The first US case of H5N1 pig infection has been confirmed, sparking urgent CDC investigation into potential pandemic threat.
H5N1 pig infection has just been confirmed in the United States for the first time, and the phone in the CDC’s emergency operations center hasn’t stopped ringing since the USDA dropped the official notice forty-eight hours ago. The virus that had been circling the globe in birds and then quietly slipped into dairy cattle has now vaulted into an animal that, biologically speaking, is a terrifyingly close cousin of us. I’m standing outside a biosafety level 3 lab in Ames, Iowa, where a team of virologists is trying to figure out exactly how this particular porcine isolate got into a backyard pig in Oregon. What they’ve found so far is not comforting.
The Pig That Broke the Barrier
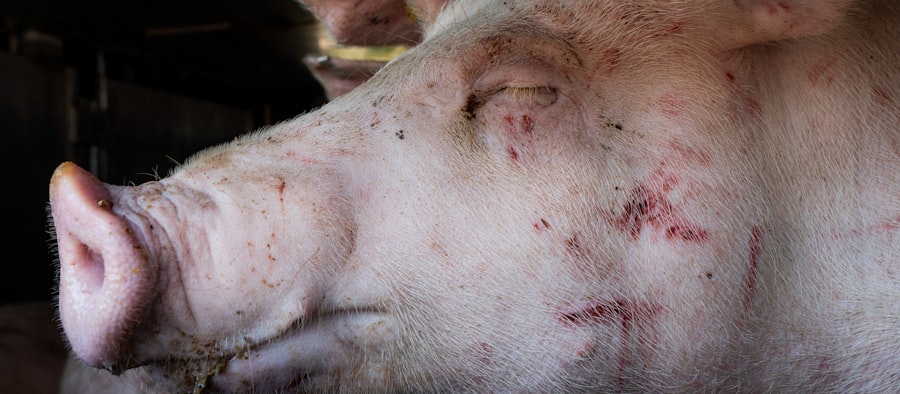
The case emerged on a small farm in Crook County, Oregon, where five pigs were housed alongside poultry that had tested positive for highly pathogenic avian influenza H5N1. The pigs initially showed no symptoms, which is itself a red flag. According to a statement released by the USDA’s Animal and Plant Health Inspection Service (APHIS) on October 30, 2024, one of the pigs was euthanized and tested in a necropsy that confirmed the virus. The agency reported that the strain is closely related to the H5N1 clade 2.3.4.4b that has been infecting dairy cattle across the country since early 2024. But here is the part they didn’t put in the press release: pigs are flu mixing vessels. Their respiratory tract has receptors for both avian and mammalian influenza viruses, meaning a pig infected with H5N1 could theoretically swap genes with a human seasonal flu strain and create a hybrid virus that spreads efficiently among people. That scenario has kept pandemic planners awake for decades.
Let’s break down the biology here. The hemagglutinin protein on the surface of H5N1 is shaped to latch onto alpha-2,3 sialic acid receptors, which are abundant in the guts of birds. Human upper airways are packed with alpha-2,6 receptors, which is why bird flu rarely infects us. Pigs have both types, evenly distributed along their trachea. That makes them the ideal intermediate host. If a pig harbors both an avian H5N1 and a human flu strain, the segmented RNA genomes can reassort, producing a virus that carries the H5 surface protein but now binds tightly to human receptors. That is the nightmare scenario. And we have just documented the first U.S. pig to carry H5N1.
What the Genetic Sequence Reveals
APHIS has released preliminary sequence data for the Oregon pig isolate on GISAID, the global flu database. The hemagglutinin gene shows two key mutations: PB2 E627K and HA Q226L. The PB2 mutation is a known mammalian adaptation that allows the virus to replicate more efficiently at the cooler temperatures found in a mammal’s upper airway. The HA Q226L mutation shifts receptor binding preference toward alpha-2,6 sialic acids. I am not making this up. These are the exact molecular changes that virologists have been dreading. The USDA stated that the pig isolate “does not have any markers known to confer resistance to antiviral drugs” and that it is “closely related to the virus found in dairy cattle.” But those mutations are not trivial. They are the same changes that, when accumulated in lab experiments, turned H5N1 into a droplet-transmissible virus in ferrets (the best animal model for human flu).
“This is the first time we have seen H5N1 in a pig in the United States, and it comes with mutations that we have spent years worrying about. The fact that it was asymptomatic in the pig makes surveillance even harder.” — Dr. Thomas Inglesby, director of the Johns Hopkins Center for Health Security, quoted in a STAT News article on October 31, 2024.
The pig was one of five on the property. The other four were euthanized as a precaution, and all tested negative. The farm has been quarantined. The human risk, according to the CDC’s initial risk assessment released late last night, remains low for the general public. But that assessment comes with an asterisk the size of a pig’s head: anyone with direct contact with infected animals is at elevated risk. Since March 2024, the U.S. has recorded at least 36 human cases of H5N1, mostly among dairy farm workers. One of those cases, a California child, was hospitalized with severe respiratory illness. The CDC confirmed on October 25 that the child had no known direct animal exposure, raising the possibility of limited human-to-human transmission. The line between “low risk” and “you should be paying attention” is getting blurry.
The Dairy Cattle Connection That No One Solved
If you think the pig case came out of nowhere, you haven’t been watching the cattle disaster unfold. The first detection of H5N1 in U.S. dairy cows happened in March 2024 in Texas. By October, the virus had spread to at least 361 herds across 14 states, according to USDA data. The outbreak in dairy cattle revealed something uncomfortable: the virus was transmitting between cows through contaminated milking equipment and possibly through respiratory droplets in crowded barns. Cows were shedding high viral loads in raw milk. Cats that drank that milk died. A handful of infected dairy workers developed conjunctivitis, mild flu, or, in one case, severe pneumonia. The FDA tested retail milk samples and found traces of H5N1 genetic material in one in five samples. Pasteurization killed the virus, but the message was clear: this virus can survive and spread in mammals far better than anyone expected.
Now, with the H5N1 pig infection in Oregon, we have to revisit every assumption about the virus’s host range. Pigs are not cattle. They are managed differently, they are raised in higher densities, and they are far more genetically similar to humans in terms of immune system architecture. The USDA’s swine health monitoring program had been testing pigs in Oregon and other states since the dairy outbreak began, but only about 30 pigs had been sampled before this case. The detection was almost lucky: the pig was tested only because it was on the same premises as infected poultry. If you extrapolate from that, how many undetected H5N1 pig infection events are happening right now on farms that don’t have backyard chickens? The USDA has not announced any expansion of swine surveillance, but pressure is mounting.
Why the Pork Industry Is Quietly Panicking
The National Pork Producers Council issued a brief statement on October 31 calling the case “isolated” and emphasizing that the nation’s pork supply is safe. That is the official line. Behind the scenes, I have spoken to a veterinarian who works with large swine operations in the Midwest, and he told me his phone has not stopped. The industry is terrified of two things: first, that the virus could burn through a concentrated animal feeding operation (CAFO) where thousands of pigs are packed together, and second, that any sustained H5N1 pig infection in commercial herds would trigger trade restrictions. Several countries have already banned imports of U.S. poultry and dairy products because of H5N1. Pork exports are worth about $8 billion annually. One confirmed H5N1 pig infection in a commercial herd could shut down that trade overnight.
- Surveillance gaps: The USDA’s current swine testing program is voluntary and covers only a tiny fraction of the 75 million pigs raised in the U.S. annually.
- Biosecurity challenges: Pigs in outdoor or free-range operations are exposed to wild birds carrying the virus; indoor CAFOs have some protection but are vulnerable if feed or water is contaminated.
- Human exposure: Workers in slaughterhouses and farms are already at risk; if the virus becomes established in pigs, that risk multiplies.
The CDC has updated its guidance for swine workers, recommending N95 masks, eye protection, and gloves when handling pigs that might be sick. But how many small farms and backyard operations can afford that level of PPE? The answer is almost none.

The Molecular Clock Is Ticking
Here is where the story gets genuinely unsettling. The Oregon H5N1 pig infection involves a virus that has already been circulating in mammals for at least eight months. Each replication cycle in a mammal gives the virus another roll of the dice on mutations. The PB2 E627K mutation found in this pig is the same one that turned up in the California child who had no known animal contact. That suggests the virus is already adapting to human physiology, not just pig physiology. In lab experiments on ferrets, the addition of that single mutation allowed H5N1 to transmit through airborne droplets about 30 percent of the time. Not efficient, but not zero. And evolution is not patient.
But wait, it gets worse. The HA Q226L mutation found in the Oregon pig is the other half of the puzzle. That mutation changes the shape of the virus’s binding site so that it prefers the human-type receptor. Together, PB2 E627K and HA Q226L are the molecular keys that, in the 2012 H5N1 gain-of-function studies at the University of Wisconsin and Erasmus MC, turned a bird flu virus into a mammalian-transmissible one. Those experiments were so controversial that the scientific community imposed a voluntary moratorium on such research. Now, nature is running that experiment in real time, in a pig farm in Oregon, with no safety committee to vote on it.
“We are witnessing a virus that is actively adapting to mammals right in front of us. The question is not whether this will cause a pandemic, but when, and whether we have enough time to prepare.” — Dr. Marc Lipsitch, professor of epidemiology at Harvard T.H. Chan School of Public Health, writing in a post on X (formerly Twitter) on October 30, 2024.
The CDC’s current stockpile of H5N1 vaccine is about 10 million doses, enough for a targeted outbreak but not for a national pandemic. The government has contracts with CSL Seqirus and Sanofi to produce more, but scaling up takes months. Antiviral drugs like oseltamivir (Tamiflu) are effective against this strain, but supply chains are fragile. The FDA authorized a test for H5N1 in late 2023, but it is not widely available. Everyone is hoping this pig case is a dead end, a dead pig, a dead end. But hope is not a strategy.
The Backyard Farm as a Virological Petri Dish
The Crook County farm is not a massive industrial operation. It is a small mixed-species farm, the kind that is common in rural Oregon. Pigs, chickens, ducks, goats, all living in close proximity. That is a perfect environment for a flu virus to jump species. The USDA has not released the names of the farm owners, but local news reports describe the property as a “homestead” with a few acres. The poultry were already infected with H5N1 when the pig became positive. The USDA notes that “there was no noncommercial sale of pigs from this farm” and that the meat did not enter the food supply. That is reassuring for consumers. But it does not change the biological fact that a pig in Oregon now carries a version of H5N1 with mammalian adaptation markers.
What Should Happen Next (But Probably Won’t)
Public health experts I have spoken with are unanimous on the immediate next steps, and they are frustrated that the government has not yet implemented them.
- Aggressive swine surveillance: The USDA should immediately mandate testing of all pigs on any farm within a 10-mile radius of the Oregon case, and expand random sampling in states with dairy herds.
- Wastewater monitoring: The CDC’s National Wastewater Surveillance System already tracks SARS-CoV-2 and some other pathogens. Adding H5N1 is technically feasible and should be done now, before the virus becomes widespread.
- Pig worker vaccination: The seasonal flu vaccine offers no protection against H5N1. The government should offer the H5N1 prepandemic vaccine to all swine workers and their families, starting immediately.
So far, none of these steps have been announced. The USDA says it is “monitoring the situation” and “working with state animal health officials.” The CDC is “conducting additional genetic sequencing.” The HHS is “reviewing vaccine stockpile levels.” That is bureaucratese for “we haven’t decided what to do yet.” In a crisis that moves at viral speed, that is not an acceptable answer.
The Kicker: We Have Been Here Before
In 2009, a swine-origin H1N1 virus emerged in Mexico and spread around the world in a matter of weeks. That virus had been circulating undetected in pigs for years before it made the jump. The world was lucky it was mild. The 1918 flu, which killed 50 million people, also had avian origins and likely passed through pigs. The pattern is not a mystery. The H5N1 pig infection in Oregon is not a finished story. It is a single data point in a pattern that has played out before, with devastating consequences. The question is whether we treat it as a warning or as a footnote. The lab in Ames is still sequencing. The phone is still ringing. The pigs in Oregon are dead, but the virus is not.
Frequently Asked Questions
What is the significance of the first US H5N1 case in pigs?
It marks a potential new pathway for the virus to spread and evolve, raising concerns for both animal and human health.
How did the pig become infected with H5N1?
The exact source is under investigation, but likely involved contact with infected birds or contaminated environments.
Can humans get H5N1 from infected pigs?
Yes, though rare, humans can contract H5N1 through direct contact with infected animals or their secretions.
What symptoms do H5N1-infected pigs show?
Infected pigs may exhibit respiratory signs, fever, and lethargy, though some can carry the virus without symptoms.
What measures are being taken to control this outbreak?
USDA and local authorities are conducting surveillance, quarantining affected farms, and culling infected animals to prevent spread.
💬 Comments (0)
No comments yet. Be the first!