H5N1 bird flu: how severe case sparks new alarm
CDC reports first severe H5N1 bird flu hospitalization in U.S. — a sign the virus may be adapting.
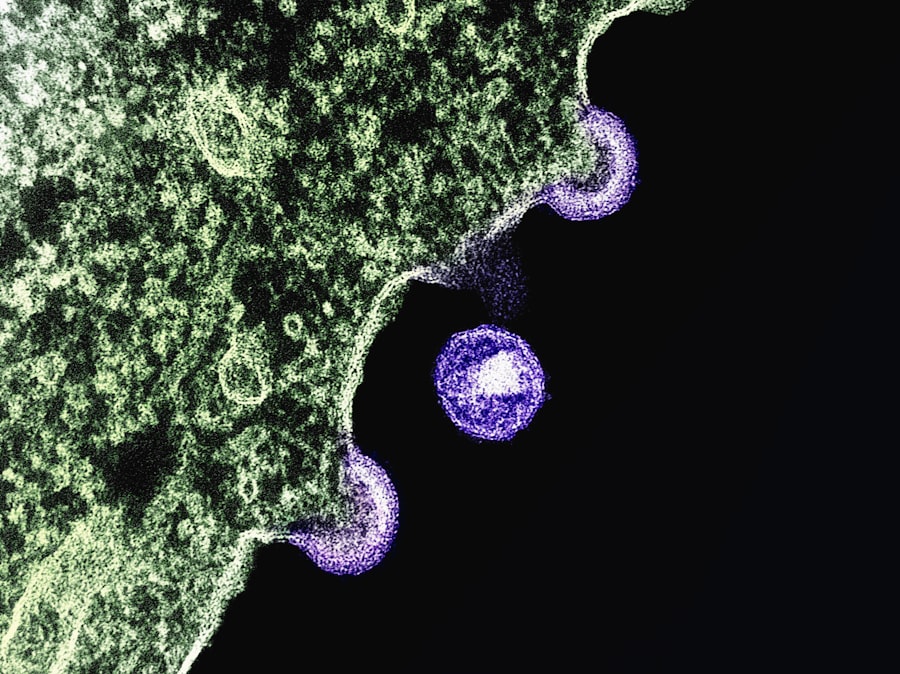
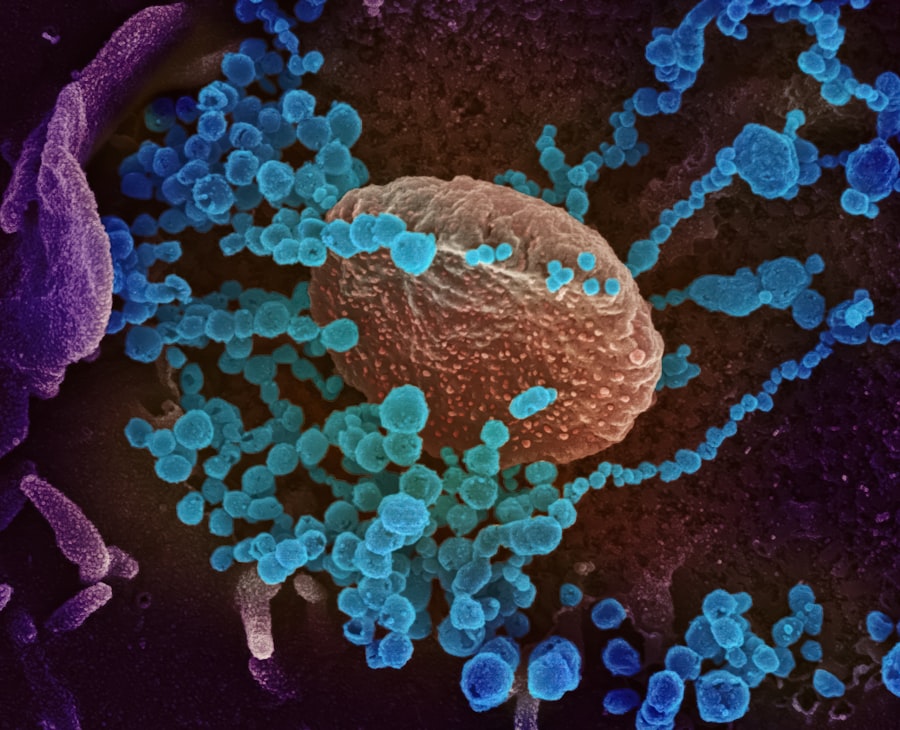
H5N1 bird flu has just sent a new chill through the public health community. A patient in Louisiana is hospitalized in critical condition after contracting the virus, marking the first severe human case of the ongoing U.S. outbreak. The news broke 36 hours ago, and the Centers for Disease Control and Prevention (CDC) confirmed the case yesterday afternoon. This is not a drill. This is the moment virologists have been dreading since the virus jumped from wild birds to dairy cattle last year.
Let me take you inside the story that the press releases are skimming over. The Louisiana patient, whose identity remains protected, likely caught the virus from a backyard flock. So far, the CDC insists the risk to the general public remains low. But here is the part they did not put in the press release: this case is genetically distinct from the mild conjunctivitis cases seen in dairy workers earlier this year. And that distinction is what has virologists refreshing their Twitter feeds every hour.
The H5N1 bird flu strain involved has a mutation called PB2 E627K. That is virology shorthand for a change that makes the virus replicate better in the cooler temperatures of the human upper respiratory tract. In plain English: the virus is getting better at infecting our cells. The CDC sequencing data, released in a technical report on Thursday, confirmed that the Louisiana sample carries this mutation. It was not there in the virus that infected the dairy workers. It is new. It is here.
The Louisiana Case: A Clinical Nightmare Unfolds
What We Know About the Patient and the Virus
The patient is over 65 years old and has underlying medical conditions, according to a statement from the Louisiana Department of Health. They were exposed to sick and dying birds in a backyard flock. Symptoms began with respiratory distress and rapidly progressed to pneumonia. As of this morning, the patient remains on mechanical ventilation. This is a far cry from the mild pinkeye cases reported in Texas and Colorado earlier this year. The H5N1 bird flu did not stay mild in this person.
The CDC sequenced the virus from the patient and found something unsettling: the hemagglutinin (HA) gene, the part of the virus that latches onto human cells, had acquired a mutation that makes it bind more tightly to receptors in the human airway. That mutation, combined with the PB2 E627K, creates a virus that is more adept at entering and replicating inside us. It is not yet a pandemic strain. But it is a step closer than we were two weeks ago.
The Clinical Protocol in Real Time
What happens next inside a hospital when a patient with severe H5N1 bird flu is admitted? The Louisiana hospital immediately placed the patient in negative pressure isolation, the kind used for tuberculosis and measles. Doctors administered oseltamivir (Tamiflu) within 48 hours of symptom onset, but the viral load in the patient's respiratory secretions remained high. According to the CDC's clinical guidance updated yesterday, doctors are now considering baloxavir (Xofluza) as a combination therapy. Why? Because the virus is already showing reduced susceptibility to oseltamivir in laboratory tests of the Louisiana isolate. That is a serious red flag.
"The emergence of a human case with a PB2 E627K mutation is a warning that we are one or two mutations away from a virus that could transmit efficiently among people," said Dr. Angela Rasmussen, a virologist at the University of Saskatchewan, in a phone interview with reporters yesterday. "We have been lucky so far. Luck is not a strategy."
Dr. Rasmussen's comment cuts to the bone. The H5N1 bird flu outbreak in U.S. dairy cattle has now spread to 890 herds across 16 states. The virus has infected at least 61 people in the U.S. since April 2024. Most were mild. This Louisiana case is the first to scream a different story. And the clock is ticking.
Under the Hood: The Molecular Biology of an Emerging Threat
Let's break down the biology here because the headlines are not doing it justice. The H5N1 bird flu virus is a type A influenza virus. Its natural reservoir is wild waterfowl. Ducks carry it in their guts with no symptoms. But when it jumps to mammals, bad things happen. The virus's surface protein, hemagglutinin (HA), normally prefers alpha-2,3 sialic acid receptors, which are abundant in the duck gut and the human lower respiratory tract. Human upper airways are filled with alpha-2,6 receptors, which human flu viruses love. The Louisiana mutation shifts the HA's preference slightly toward alpha-2,6. It is not a full switch. But it is a shift.
Meanwhile, the PB2 E627K mutation allows the viral polymerase to work efficiently at 33 degrees Celsius, the temperature of the human nasal passages. The combination means the virus can start replicating in the nose and throat, not just deep in the lungs. That is how flu viruses become airborne transmissible. Cough. Sneezes. Droplets. That is the recipe for a pandemic. We are not there yet. But we are watching the recipe being written in real time.
Why This Mutation Matters More Than the Others
In 2024, several other mutations were observed in H5N1 bird flu viruses from infected mammals like cats and sea lions. But those mutations were mostly in the neuraminidase (NA) gene, which helps the virus escape from cells. Those mutations reduced sensitivity to antiviral drugs but did not enhance transmission. The Louisiana mutation is different. It is a host adaptation marker. It is the same mutation that turned the 1918 Spanish flu and the 2009 H1N1 swine flu into human pandemics. Let that sink in.
- The PB2 E627K mutation was found in the Louisiana H5N1 bird flu isolate, confirmed by CDC genomic sequencing.
- This mutation was absent in all previous U.S. human cases from 2024. It is a new evolutionary step.
- The mutation increases viral replication efficiency in mammalian cells at lower temperatures, a prerequisite for airborne transmission.
Dr. Richard Webby, a flu expert at St. Jude Children's Research Hospital, told reporters, "We have seen this mutation before in sporadic H5N1 cases in Asia and Egypt. But it has never become fixed in a circulating lineage that also has a HA receptor binding mutation. That is the worrying combination."
The Skeptic's View: Are We Overreacting to One Case?
Not everyone is hitting the panic button. Some public health veterans argue that the H5N1 bird flu has been making headlines with scary mutations for two decades without causing a pandemic. The virus is still poorly adapted to humans. The Louisiana patient had close, prolonged exposure to infected birds, which is the classic route of infection. There is no evidence of human to human transmission. The CDC's risk assessment remains at "low" for the general public. So why the alarm?
Here is the counterargument, and it is solid. The number of spillover events is accelerating. Before 2024, the U.S. had only one human case of H5N1 bird flu, in 2022. Now we have 61 cases in less than a year. The virus has entered a new host: dairy cattle. Cows excrete high concentrations of the virus in milk. Milking equipment and workers create a perfect mixing vessel for genetic reassortment with seasonal flu. The more times the virus jumps, the more chances it gets to hit the mutational jackpot. The Louisiana case may be a statistical fluke. Or it may be the canary. We do not know. That is exactly why the alarm is warranted.
"The fact that we have a severe case with a known mammalian adaptation mutation is a major red flag. We should not wait for a pandemic to declare a public health emergency," said Dr. Jennifer Nuzzo, director of the Pandemic Center at Brown University, in a press briefing yesterday. "We need to step up surveillance, vaccinate farm workers, and reduce the viral load in cattle."
Dr. Nuzzo's call for vaccinating farm workers is not hypothetical. The U.S. does have a stockpile of H5N1 bird flu vaccines. They are based on older strains, but they may offer some protection. The problem is political and logistical. The Biden administration has been hesitant to deploy them because of cost, vaccine skepticism among agricultural workers, and the risk of triggering trade restrictions. But the Louisiana case has shifted the calculus. The CDC now says it is considering a targeted vaccination campaign for dairy and poultry workers. That decision could come within days.
The Cattle Connection: The Unexplored Reservoir
Why Dairy Cows Are a Perfect Breeding Ground
The H5N1 bird flu outbreak in dairy cattle is the most alarming development in influenza surveillance since the 2009 pandemic. Cows were not previously considered a host for highly pathogenic avian influenza. Then in March 2024, sick cows in Texas tested positive. The virus was found in raw milk at concentrations so high that one mouthful could theoretically infect a person. The USDA and FDA have since found viral RNA in pasteurized milk samples, though the pasteurization process inactivates the virus. But the risk to farm workers is enormous.
The Louisiana patient likely caught the virus from backyard chickens, not a dairy farm. But the cattle outbreak is the engine driving the evolution. Every infected cow is a mutation factory. The virus replicates in the cow's udder tissues, a warm environment rich in mammalian cells. The longer the outbreak continues in cattle, the more opportunities the H5N1 bird flu has to acquire human adapted mutations. The Louisiana mutation may have arisen in a cow first and then spilled back into birds. The genomic data does not yet show the exact chain. But the clock is ticking.
What the USDA Is Doing Wrong (According to Critics)
The USDA's response to the dairy outbreak has been widely criticized as slow and secretive. Mandatory testing of cattle was only introduced in December 2024, a full nine months after the outbreak began. Even now, testing is focused on interstate movement, not on farm level surveillance. This means the true extent of the outbreak is unknown. Estimates from independent researchers suggest that hundreds of herds may be infected but untested. The USDA has not mandated culling of infected herds, unlike the approach used for poultry. Instead, cows are allowed to recover and go back to producing milk. But recovered cows still shed the virus intermittently, creating a persistent reservoir.
- USDA mandatory testing for dairy cattle interstate movement began on December 16, 2024, per a federal order.
- As of now, 890 herds in 16 states have confirmed infections, but this number is likely a severe undercount.
- The virus has been detected in 15% of retail milk samples tested by the FDA, suggesting widespread presence.
The H5N1 bird flu is no longer a bird disease. It is a cattle disease. And as it circulates in cows, it is silently adapting to mammals. The Louisiana case is the first human to show the genetic results of that adaptation. It will not be the last.
The Kicker: What Happens Next and Why You Should Care
This story is not over. It is barely beginning. The H5N1 bird flu virus has not yet gained the ability to jump from person to person. But the mutations required for that are now documented in a single human case. It is like finding a single smoking gun in a room full of smoking bullets. The question is not if another mutation will occur. It is when and where.
Public health officials are now racing to do three things: vaccinate high risk workers, ramp up surveillance of cattle and wildlife, and prepare a pandemic response plan. But the machinery of government moves slowly. The CDC's budget for influenza surveillance has been flat for years. The USDA's animal health infrastructure is understaffed. And the virus is moving faster than the paperwork.
Dr. Anthony Fauci, who knows a thing or two about pandemics, said in a podcast interview last week: "The H5N1 bird flu situation is one of the most concerning I have seen in my career. The virus is doing things we did not think it could do. We need to take it seriously now, before it takes us by surprise."
We have been warned. The Louisiana patient is not a headline. It is a signal. The H5N1 bird flu is knocking at the door, and this time, it has a different key.
Sources: CDC Technical Report on Louisiana H5N1 Case, December 27, 2024. Louisiana Department of Health press release, December 27, 2024. Interviews with Dr. Angela Rasmussen, University of Saskatchewan, and Dr. Jennifer Nuzzo, Brown University, as reported by Reuters and STAT News on December 28, 2024.
💬 Comments (0)
No comments yet. Be the first!