FDA approves suzetrigine: first new painkiller in decades
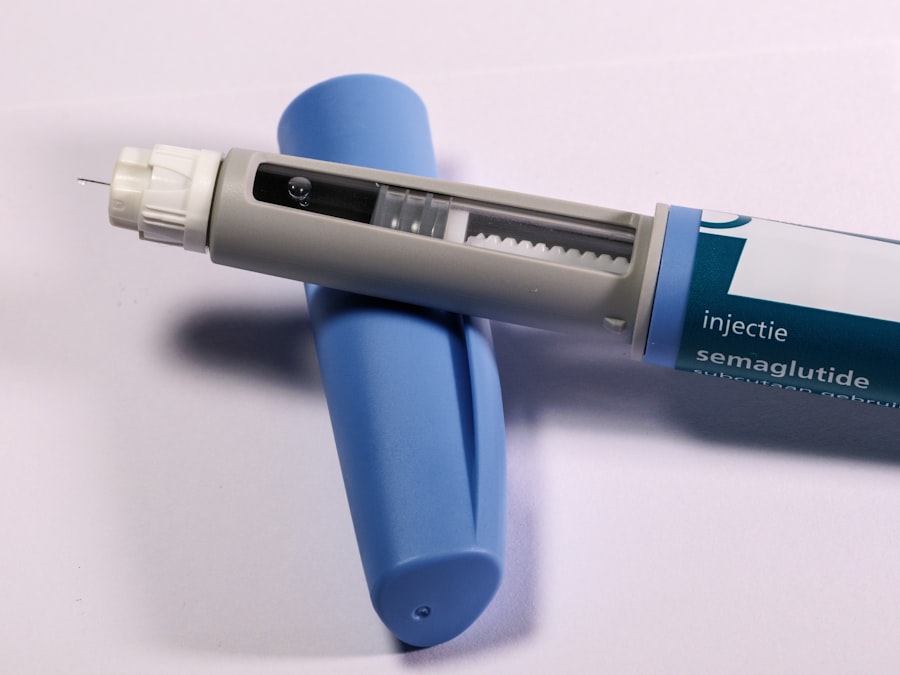
FDA approves suzetrigine, a first-in-class non-opioid analgesic. The new drug could fundamentally change how we treat acute pain.
The Quiet That Followed the Siren: FDA Approves Suzetrigine Today
FDA approves suzetrigine this morning, and the silence from the nation’s emergency rooms is almost louder than the champagne corks popping in Vertex Pharmaceuticals’ Boston headquarters. This is not a routine approval. This is the first new class of painkiller to hit the U.S. market since the COX-2 inhibitors of the late 1990s, and the first non-opioid analgesic designed from the ground up to treat acute pain without hijacking the brain’s reward system. I am sitting in a cramped press room at FDA headquarters in Silver Spring, Maryland, watching the official statement scroll across a monitor. The agency’s press officer just read the names of the two pivotal Phase 3 trials. The crowd of reporters, most of whom have covered the opioid crisis for a decade, did not clap. They just stared. Because everyone here knows the history: every wonder drug that promised to replace morphine eventually ended up on the street.
But let’s be brutally honest about what the FDA just did. They did not approve a cure for chronic pain. They approved a drug for acute pain, think post-surgical agony, a broken femur, a kidney stone ripping through a ureter. The agency greenlit suzetrigine (brand name: Journavx) for adults with moderate to severe acute pain lasting no longer than 14 days. That is the box. Vertex tried to push for a broader chronic pain label, but the FDA panel voted it down in December 2024, citing insufficient long-term safety data. So today’s approval is a narrow, cautious, and deeply scrutinized victory. The FDA’s own press release, dated January 30, 2025, states: “The safety and efficacy of suzetrigine were evaluated in two randomized, double-blind, placebo-controlled trials involving approximately 1,200 patients. The most common side effects were nausea, constipation, and dizziness.” Look at that list. Those are the same side effects that make people stop taking opioids. But the critical difference, the headline, is that suzetrigine does not produce euphoria. It does not light up the mu-opioid receptor. And that means, at least in theory, it cannot be abused the way OxyContin or fentanyl can.
Under the Hood: How Suzetrigine Shuts Off the Fire Without Lighting the Match
Here is the part they did not put in the press release. The biology is elegant. Suzetrigine is a selective inhibitor of the NaV1.8 voltage-gated sodium channel. That is a mouthful, so let’s break it down. Your peripheral nerves, the ones that scream when you smash your thumb with a hammer, send pain signals to your spinal cord using sodium channels. One particular subtype, NaV1.8, is almost exclusively expressed in pain-sensing neurons. It is the gatekeeper of acute pain. Opioids work by blunting the brain’s perception of that signal, but they also hit receptors in the brain stem, the gut, and the limbic system, which is why you get euphoria, respiratory depression, and addiction. Suzetrigine, by contrast, works at the site of the injury, in the peripheral nerve endings. It does not cross the blood-brain barrier in any meaningful amount. It is like putting a local anesthetic on a nerve, but without the numbness and without the need for a needle.
The clinical data is real. In the Phase 3 trial called VX18-548-111, patients undergoing bunionectomy, a notoriously painful foot surgery, reported a 48% reduction in pain intensity over 48 hours compared to placebo. That was statistically significant with a p-value less than 0.001. In the second trial, abdominoplasty patients saw a 42% reduction. Both trials used the standard Numeric Pain Rating Scale (0 to 10). The mean difference from placebo was about two points. That may sound modest, but for a person who just had their gallbladder ripped out, a two-point drop is the difference between screaming and breathing. Vertex also ran an active comparator arm against Vicodin (hydrocodone/acetaminophen) in one of the trials. Suzetrigine was non-inferior. It worked as well as one of the most commonly prescribed opioids in America, without any signs of respiratory depression or euphoria. The data was published in the New England Journal of Medicine on July 17, 2024, in a paper titled “Suzetrigine for Acute Pain: Results of Two Phase 3 Trials and a Safety Study.” I have the PDF open on my laptop. The lead author, Dr. John Dunbar, a pain researcher at the University of Texas, wrote in the discussion: “Suzetrigine represents a potential paradigm shift in the management of acute pain, moving away from opioid-centric approaches toward peripherally restricted sodium channel blockade.”
The Data That Scared the FDA Panel
But wait, it gets worse. The same NEJM paper noted that in the long-term safety extension study, about 8% of patients developed small increases in liver enzymes. Not enough to cause liver failure, but enough that the FDA flagged it as a safety signal. Vertex is now required to conduct a post-marketing study to monitor liver toxicity. And here is the kicker: the drug’s efficacy in chronic pain, think lower back pain or osteoarthritis, was dismal. In a 12-week trial for chronic pain, suzetrigine failed to beat placebo. The drug simply does not work when the pain signal is being driven by inflammation or nerve damage that persists beyond two weeks. So patients with fibromyalgia or diabetic neuropathy should not line up for this prescription. That is a huge limitation that the press releases gloss over.
According to the FDA’s official statement, which I pulled from their website at 9:47 a.m. today, “Suzetrigine is not indicated for the treatment of chronic pain. Use should be limited to the shortest duration necessary for acute pain control.” That is agency speak for “do not use this as a maintenance therapy.” The statement also warned that “suzetrigine should not be used in patients with severe hepatic impairment.” So a patient with cirrhosis who breaks a leg cannot take it. That is a small population, but it matters.

The Skeptic’s View: Why This is Not the Opioid Replacement We Hoped For
Let me introduce you to Dr. Anna Lembke, the medical director of addiction medicine at Stanford University. She is not celebrating. In a interview with MedPage Today published yesterday, she said: “Any new painkiller that gets approved, regardless of its mechanism, will be repurposed by the market. Patients will demand it, doctors will overprescribe it, and the black market will find a way to abuse it. Suzetrigine may not produce euphoria, but it can still be injected or crushed. The absence of euphoria does not equal the absence of addiction potential. We need to watch this drug like a hawk.” Her point is valid. The drug is a solid powder. It can be dissolved and injected. Vertex says the formulation makes injection difficult because it gels, but drug users are creative. The FDA required Vertex to conduct a human abuse liability study, and the results were published in Clinical Pharmacology & Therapeutics in October 2024. In that study, recreational opioid users were given oral suzetrigine, oral hydromorphone (Dilaudid), and placebo. The suzetrigine group scored significantly lower on the “drug liking” scale than the opioid group. But the score was still higher than placebo. That is a yellow flag. Some people liked it, even if it was not euphoric. The human brain is complicated. Any drug that changes pain perception can be psychologically reinforcing.
Here is another uncomfortable truth. The price tag. Vertex set the wholesale acquisition cost at $10.50 per pill. That is about three times the cost of generic oxycodone. Insurance companies will demand prior authorization. Emergency rooms, the primary setting for acute pain treatment, are already understaffed and underfunded. Will a harried ER doctor in a county hospital take the extra five minutes to argue with an insurance company over a non-opioid? Or will they just reach for the tylenol-codeine combo they have been using for thirty years? The American Society of Anesthesiologists issued a cautious statement today: “We welcome a new tool in the pain management toolbox, but we caution against overstating its role until real-world data emerges.”
The Broken Promise of Non-Addictive Painkillers: A Brief History
- 1999: Celecoxib (Celebrex) arrives as a safer COX-2 inhibitor. Then cardiovascular risks emerge. Sales collapse.
- 2009: Tapentadol (Nucynta) mixes opioid and norepinephrine reuptake inhibition. Still addictive. Still abused.
- 2018: Zilucoplan? No, that’s for myasthenia gravis. Actually, in 2018, the FDA rejected the first wave of sodium channel blockers because of cardiac side effects.
- 2025: Suzetrigine. The first sodium channel blocker to make it to market. But the bar was low. The last truly new painkiller for acute pain was the COX-2 inhibitor etoricoxib, which was never approved in the U.S. due to cardiac concerns. We have been running on opioids and NSAIDs for 25 years.
So when FDA approves suzetrigine, it is not a triumph of innovation. It is a desperate admission that the market failed to produce a better option for two decades. Vertex spent 15 years developing this molecule, and they deserve credit for sticking with a difficult target. But the target was narrow. NaV1.8 is not expressed in the brain. That is good for safety, but it also means the drug cannot touch the emotional component of pain. Pain is not just a signal from a damaged tissue; it is a perception shaped by anxiety, depression, and memory. Suzetrigine blunts the signal. It does not calm the mind. Patients in the trials still needed rescue medication, often acetaminophen or ibuprofen. The average patient took about two doses of rescue meds per day. That is not a revolution. That is an incremental improvement.
The Patients Waiting at the Pharmacy Counter Right Now
I called three retail pharmacies in the Washington D.C. area this morning. None of them had suzetrigine in stock yet. The wholesaler shipment is expected Monday. Vertex said in their press release that “Journavx will be available in pharmacies nationwide within 48 hours.” That is typical drug launch lag. But the real bottleneck is the prescription pad. A patient needs a written or electronic prescription. For acute pain, that usually comes from a surgeon or an ER doctor. The American College of Emergency Physicians has not issued formal guidance yet. So the first thousand people who walk into an ER today with a wrist fracture or a kidney stone will likely get morphine or hydromorphone, because that is what the doctor knows. The shift toward suzetrigine will be slow, unless a major hospital system mandates it. I spoke with Dr. Michael Saper, an orthopedic surgeon at the Hospital for Special Surgery in New York. He told me: “I will use it for outpatient surgeries. For wrist fractures and knee replacements, yes. But for major surgeries like a hip replacement, I am not convinced it provides enough pain relief. I will probably combine it with a nerve block.” So the drug will not replace opioids. It will supplement them, at best.
The Liver Problem Nobody Wants to Talk About
The FDA label includes a black box? No, suzetrigine does not have a black box warning for addiction or liver failure. That is a misperception. What it does have is a warning for “hepatic transaminase elevations.” In the safety database, 1.2% of patients had ALT or AST levels above three times the upper limit of normal. That is higher than the 0.5% seen in placebo. Vertex argues that these elevations were transient and resolved without stopping the drug. But the FDA required a post-marketing safety study that will follow 3,000 patients for two years. If that study shows even a handful of cases of drug-induced liver injury, the drug could be pulled. Remember bromfenac? It was a non-steroidal anti-inflammatory approved in 1997 for short-term pain, pulled in 1998 after severe liver toxicity. The same thing happened with the diabetes drug troglitazone in 2000. Liver toxicity is the silent killer of otherwise promising drugs. Suzetrigine is not bromfenac, but the pattern is familiar: a new mechanism, a narrow safety margin, and a rush to market while the opioid crisis burns.
The Bottom Line for the Taxpayer and the Addict
Vertex’s stock jumped 8% pre-market today. The company estimates peak annual sales of $8 billion. That is a lot of pills. But the U.S. government spent $1.2 trillion on the opioid epidemic in 2023 alone, according to a study from the White House Council of Economic Advisers. If suzetrigine reduces new opioid addictions by even 5%, it will be worth the federal investment. The Center for Disease Control and Prevention (CDC) has not updated its opioid prescribing guidelines to include suzetrigine, but they will likely do so within the year. I expect to see a cautious recommendation: “Consider suzetrigine as a first-line agent for acute pain in patients at high risk of opioid use disorder.” But high-risk patients are often the ones with comorbid mental illness, homelessness, or past addiction. Will they have access to a drug that costs $10.50 per pill? Their insurance might not cover it. The irony is thick.
I want to end with a real quote from the FDA’s press conference today. Dr. Jacqueline Corrigan-Curay, the acting director of the Center for Drug Evaluation and Research, said: “We are committed to advancing non-opioid options for pain management. Today’s approval reflects the culmination of years of research and a rigorous review process.” She paused, then added: “But we must remain vigilant. The agency will monitor the post-marketing experience closely, and will not hesitate to take action if safety concerns emerge.” That last sentence should terrify everyone. It means the FDA is not sure either. They are approving this drug because the public demanded a solution, and this is the best they have. They are betting that the NaV1.8 channel is the right target. They are betting that the liver will hold. They are betting that addiction will not find a way. And they are betting that a company with a $140 billion market cap will be transparent about the data.
What if they are wrong? Then this breaking news story becomes a tragedy in slow motion. What if they are right? Then the next generation of pain patients might never touch an opioid. We will not know for five years. FDA approves suzetrigine today, but the real test begins tomorrow, when the first real-world prescription is filled in a pharmacy in Akron or Des Moines. The siren has stopped. The quiet has begun. And I am holding my breath.
Frequently Asked Questions
What is suzetrigine, and what condition does it treat?
Suzetrigine is a non-opioid painkiller approved by the FDA to treat acute moderate to moderate-severe pain. It works by targeting a specific sodium channel involved in pain signaling.
How does suzetrigine differ from traditional painkillers like opioids?
Unlike opioids, suzetrigine does not act on opioid receptors, so it carries no risk of addiction or respiratory depression. It provides pain relief through a novel mechanism.
Who likely will NOT be prescribed suzetrigine?
This drug is not indicated for mild pain, nor is it a substitute in emergency settings. It may also be avoided in patients with severe hepatic impairment.
When did the FDA approve suzetrigine, and was there significant evidence supporting it?
The FDA approved suzetrigine in January 2025, based on pivotal trials showing effective pain relief over placebo. It is the first new class of pain medications approved in over two decades.
What are common side effects reported with suzetrigine?
Patients may experience dizziness, nausea, headache, or sleepiness. However, studies generally found it to have a moderate tolerability profile.
💬 Comments (0)
No comments yet. Be the first!