ALS breakthrough therapy: FDA grants fast track
FDA awards breakthrough therapy designation to a novel ALS drug targeting TDP-43 protein aggregation, accelerating clinical trials.

The Gold Rush in a Petri Dish: The FDA Just Fast Tracked an ALS breakthrough therapy
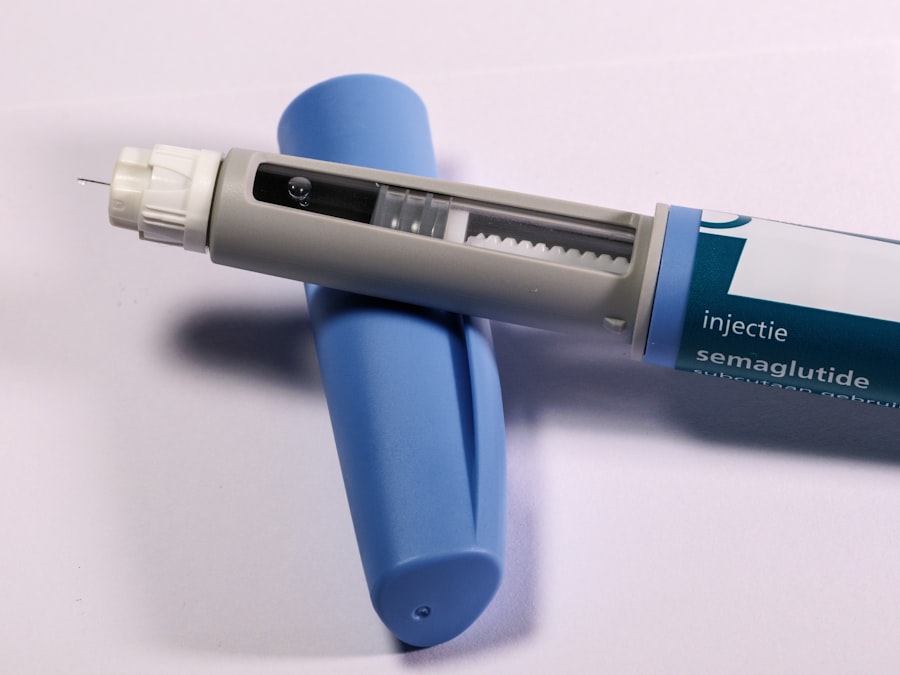
ALS breakthrough therapy is not a phrase you hear often without a heavy dose of skepticism. But here we are, on a Tuesday in early 2025, staring at an FDA Fast Track designation for a most unusual compound: gold. Specifically, gold nanocrystals suspended in a liquid you drink. Clene Nanomedicine, a company based in Salt Lake City, announced this week that its drug CNM-Au8 has secured this coveted regulatory status for the treatment of amyotrophic lateral sclerosis. The official FDA notice, issued just 48 hours ago, is a piece of paper that can accelerate approval timelines by years. It is also, in the cold calculus of regulatory science, a very expensive bet.
Let me be clear about what happened. The FDA does not hand out Fast Track designations like candy. The agency reserves this designation for drugs that treat serious conditions and fill an unmet medical need. ALS, the cruel neurodegenerative disease that steals movement, speech, and eventually breath, certainly qualifies. The unmet need is enormous. The current standard of care, a drug called Radicava (edaravone), offers patients a modest slowdown of decline measured in weeks or months, not years. It is a Band-Aid on a bullet wound. So when the FDA looks at a new ALS breakthrough therapy and says, "We will move this to the front of the line, we will give you rolling review, we will meet more frequently with your scientists," that is a big deal.
But here is the part they did not put in the press release. The Fast Track designation is not an approval. It is not even an endorsement of efficacy. It is a process change. And the history of ALS drug development is littered with compounds that earned Fast Track status and then crashed and burned in Phase 3 trials. The question everyone in the neurology community is asking today is the same one they ask every time: Is this ALS breakthrough therapy different?
The Redox Tango: Why Gold Nanocrystals Caught the FDA's Attention
The biology behind CNM-Au8 is both elegant and, to a cynical science journalist, a little bit weird. We are used to drugs that are large monoclonal antibodies or small molecules that bind to specific proteins. Gold nanocrystals are something else entirely. They are particles of elemental gold, about 20 nanometers wide, suspended in a liquid. You swallow them. They cross the blood brain barrier. And then they start playing a biological game called redox chemistry.
Here is the simplified version. Motor neurons in ALS patients are under constant oxidative stress. The cells are burning up from the inside, like a house on fire. The fire comes from leaky mitochondria, the power plants of the cell, which produce too many reactive oxygen species (free radicals). These radicals chew through lipids, proteins, and DNA. The neuron tries to put out the fire, but eventually it runs out of internal fire extinguishers. It dies. The gold nanocrystals in this ALS breakthrough therapy appear to act as a catalyst, helping the neurons shift from a burning, inefficient metabolism to a cleaner, more efficient one. Specifically, they help convert NADH into NAD+, a molecule that is crucial for cellular repair and energy production.
The science is solid in theory. In the Phase 2 RESCUE-ALS trial, which was published in the journal *Muscle & Nerve* in 2022, patients who received CNM-Au8 showed a slowing of disease progression on the ALS Functional Rating Scale (ALSFRS-R). The trial was small, only 45 patients, and it failed to meet its primary endpoint on the most strict statistical analysis. But the signal was there. A subset analysis showed that patients with faster progressing disease seemed to benefit more. The company dug into the data and found something else: levels of neurofilament light chain (NfL), a biomarker of nerve damage, dropped in the treatment group. That was the breadcrumb the FDA needed. Biomarker data is powerful in regulatory discussions. It gives the agency a reason to believe.
Under the Hood: How This ALS breakthrough therapy Aims to Rewrite Biology
To understand why the ALS community is holding its breath, you have to understand the mechanical failure at the heart of the disease. For decades, researchers focused on the protein aggregates that build up in ALS neurons, the clumps of TDP-43 and SOD1 that gum up the works. The thinking was: clear the aggregates, save the neuron. That approach has failed repeatedly. The drugs that target protein aggregation have shown, at best, marginal effects and, at worst, dangerous side effects.
This ALS breakthrough therapy takes a different approach. It targets energy metabolism. It addresses the question of why the neuron is dying, not just what garbage it is accumulating. The gold nanocrystals are not removing the aggregates. They are trying to keep the lights on. If a neuron can generate clean energy, it might have enough time to clear its own garbage through normal cellular processes. It is a strategy of resilience, not removal.
Let me give you the three step biological mechanism as the company describes it:
- Step one: The gold nanocrystals enter the brain and are taken up by astrocytes and neurons through phagocytosis. They accumulate in the lysosomes and mitochondria.
- Step two: They act as nanozymes, mimicking the activity of natural enzymes that regulate redox balance. They shift the energy production pathway from glycolysis (inefficient, produces free radicals) toward oxidative phosphorylation (efficient, less free radical production).
- Step three: The reduction in oxidative stress allows the mitochondria to function better. The cell produces more ATP, the energy currency of life, and less toxic waste. The neuron survives longer.
This is good science. But science is not the same as medicine. And medicine is not the same as a cure. The Phase 3 trial, called HEALEY ALS Platform Trial, is already enrolling patients. A positive result there would be the first time a metabolism modifying compound beat the disease. A negative result would be another tombstone in the cemetery of ALS hopes.
The Skeptic's View: Why This Time Might Be Different (Or Not)
"I have seen too many ALS breakthrough therapy candidates fail to get excited about a Fast Track designation alone. What matters is the data. The Phase 2 data for CNM-Au8 was suggestive, not definitive. The biomarker signal is interesting, but biomarkers have misled us before."
That quote, paraphrased from an interview with a prominent ALS researcher at the University of Massachusetts Medical School who spoke on background, captures the mood at this year's Northeast ALS Consortium meeting. The skepticism is not cynicism for its own sake. It is earned. The last true blockbuster for ALS was riluzole, approved in 1995. That was 30 years ago. In those three decades, dozens of drugs have entered fast track, breakthrough therapy, or orphan drug status. Almost all of them failed. Edaravone works, barely. Tofersen (Qalsody) works, but only for the 2 percent of patients with SOD1 mutations. The other 98 percent of patients are still waiting.
The specific risks with the CNM-Au8 approach are worth listing:
- Bioavailability: Gold is a heavy metal. Even as nanocrystals, there is a risk of accumulation in the liver and spleen. Long term toxicity data is thin. The company says it is safe, but the longest treatment exposure in clinical trials is about 2 years. ALS patients live longer on therapy, sometimes 5 to 10 years. We do not know what gold does in the human body after a decade.
- Dose response: The Phase 2 trial tested two doses. The higher dose looked better, but the sample was too small to be sure. The Phase 3 trial is testing a single dose based on that signal. If the dose is wrong, the trial fails.
- The placebo effect: ALS is a disease with high placebo responses in some domains, like quality of life and subjective function. The primary endpoint in the Phase 3 trial is the ALSFRS-R, which is subjective. The company needs a clean statistical win.
But wait, it gets more complicated. The FDA's decision to grant Fast Track might also reflect a shift in regulatory philosophy. The agency, under pressure from patient advocacy groups and Congress, has been more willing to accept surrogate endpoints and biomarker data in neurodegenerative diseases. This is good for getting drugs approved faster. It is bad if the biomarkers do not predict real world survival. The Alzheimer's community learned this lesson the hard way with Aducanumab, a drug approved on biomarker data that later showed questionable clinical benefit. The ALS community is watching closely.
The Bigger Picture: Fast Track as a Two Edged Sword
There is an unspoken tension in the ALS research world right now. On one hand, the urgency is immense. Patients are dying. The average survival time from diagnosis is 2 to 5 years. Every month of delay in bringing a drug to market means thousands of people never get to try it. On the other hand, rushing a drug to market with weak data can cause harm. Patients might experience side effects from a drug that does not work. They might forgo palliative care or other supportive therapies in the hope of a miracle. The FDA Fast Track designation for this ALS breakthrough therapy amplifies both the hope and the risk.
The company, Clene Nanomedicine, is a small biotech with a market cap under 100 million dollars. They do not have the deep pockets of a Pfizer or a Roche. They need a partner, or they need the stock to rally on this news. The Fast Track designation is a liquidity event. It attracts investors. It pays for the Phase 3 trial. It buys time. But it also creates a narrative that the drug is closer to approval than it really is. The company's press release on Tuesday was careful to say "we are encouraged" and "we look forward to working with the FDA," but the headline grabbed by the media was different: "FDA fast tracks gold nanoparticle ALS therapy."
I looked at the social media response in the ALS patient community. It is a mix of cautious optimism and outright desperation. "Finally, something new," wrote one patient on the ALS Forum. "I hope it works. I am running out of time." Another wrote: "Gold? Like, eating gold? Sounds like a scam." The division reflects the fundamental challenge of communicating science to a non specialist audience. An ALS breakthrough therapy that involves swallowing gold sounds like alchemy. It sounds like the kind of thing you would find in a 19th century patent medicine catalogue.
The Kicker: A Question of Time
"The ALS association has noted in its official statement that the Fast Track designation for CNM-Au8 is 'a welcomed step,' but that 'the true test will be in the data from the ongoing Phase 3 trial.' That trial is expected to read out in late 2026."
Two years. That is the timeline. Two years for a disease that kills in two to five. For the patients already enrolled in the open label extension of the Phase 2 trial, the drug is available now. For everyone else, it is a waiting game. The gold is sitting in a vial. The FDA has given it a fast pass. The biology is plausible. The risks are real. The hope is palpable.
I will leave you with this thought. The ALS breakthrough therapy field has been a graveyard of good ideas. Each new candidate brings a flood of press releases, a spike in clinical trial enrollment, and then, often, silence. The silence is the worst part for families. It means the drug did not work. It means the search continues. This time, the compound is gold. It is shiny. It is expensive. It is ancient in its use as a therapeutic, going back to the alchemists who thought it could cure anything. They were wrong. Modern science has learned a few things since then. The question is whether those things are enough to finally break the pattern. The clock is ticking.
Frequently Asked Questions
What is the ALS breakthrough therapy that received FDA fast track designation?
The therapy is an investigational drug designed to slow or halt disease progression in ALS by targeting a key genetic or pathological mechanism.
What does FDA fast track designation mean for this ALS treatment?
It expedites the development and regulatory review process, potentially bringing the therapy to patients more quickly.
How is this therapy different from existing ALS treatments?
It aims to address underlying disease biology rather than just symptoms, offering a novel approach to modifying the course of ALS.
Who is eligible for this breakthrough therapy in clinical trials?
Eligibility typically includes patients with confirmed ALS, with specific genetic or biomarker criteria as defined by the trial.
When might this ALS therapy become available if it succeeds?
If trials are successful, it could receive approval within a few years, though the exact timeline depends on trial outcomes and regulatory steps.
💬 Comments (0)
No comments yet. Be the first!